Infusion Blog
- Vascular Access
- Uncategorized
- Training
- Storytelling
- Sponsored
- Scheduling
- Risk Management
- Providers
- Press Release
- Pharmacology
- Patients
- Operations
- Legal Risk Mitigation
- Legal
- Insurance
- Infusion Patients
- In The News
- Emergency Resources
- Disease Management
- Data Management
- Chronic Illness
- Billing
- Artificial Intelligence
- Advocacy
- Access Issues
Highlights, participant insights, and what’s next after our inaugural pre-conference workshop in Miami Beach. The infusion industry is changing rapidly. As demand for biologics and specialty […]
How Verification, Validation, and Value reporting can turn GenAI pilots into sustainable operational improvements Every infusion operator I know is thinking about AI right now. There […]
Tucked away in the Centers for Medicare and Medicaid Services (CMS) CY 2026 Home Health and DMEPOS final rule, CMS finalized several updates to Medicare provider […]
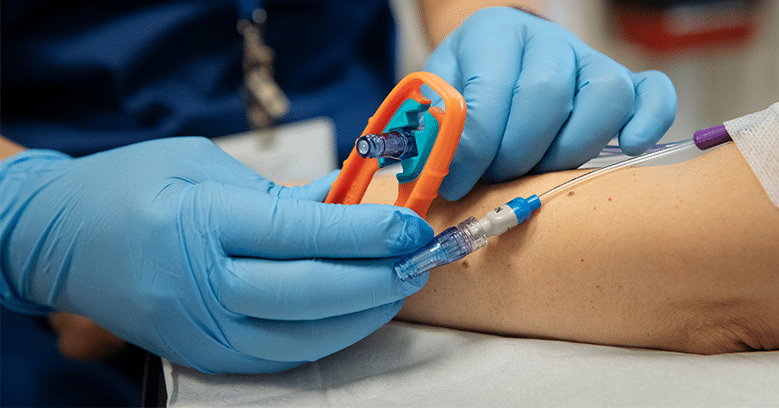
In infusion care, safety and efficiency are at the heart of everything we do. Each connection and disconnection of an IV line may seem routine, but […]
From Intake to Impact: Financial Strategies That Strengthen the Infusion Revenue Cycle A Strong Start: Why Intake Defines Financial Success In infusion and specialty care, a […]
Introduction: The Case of the Manic Monday Imagine you are the nurse manager at “ACME Infusion Center.” You arrive at the clinic early Monday morning like […]
Infusion Alphabet Soup Part 1: Understanding Infusion Delivery Models Today Originally published: June 14, 2023 Updated and reposted: August 14, 2025 By: Bryan Johnson AIC, AIS, […]
For infusion centers, a strong portfolio of health plan contracts isn’t optional—it’s the foundation of patient access, referral relationships, and sustainable growth. Being in-network with the […]
The High Cost of Keeping the IVs Dripping Operating an ambulatory infusion center means walking a financial tightrope. While the primary mission is delivering outstanding patient […]